Hip Replacement Surgery in Santa Rosa, CA
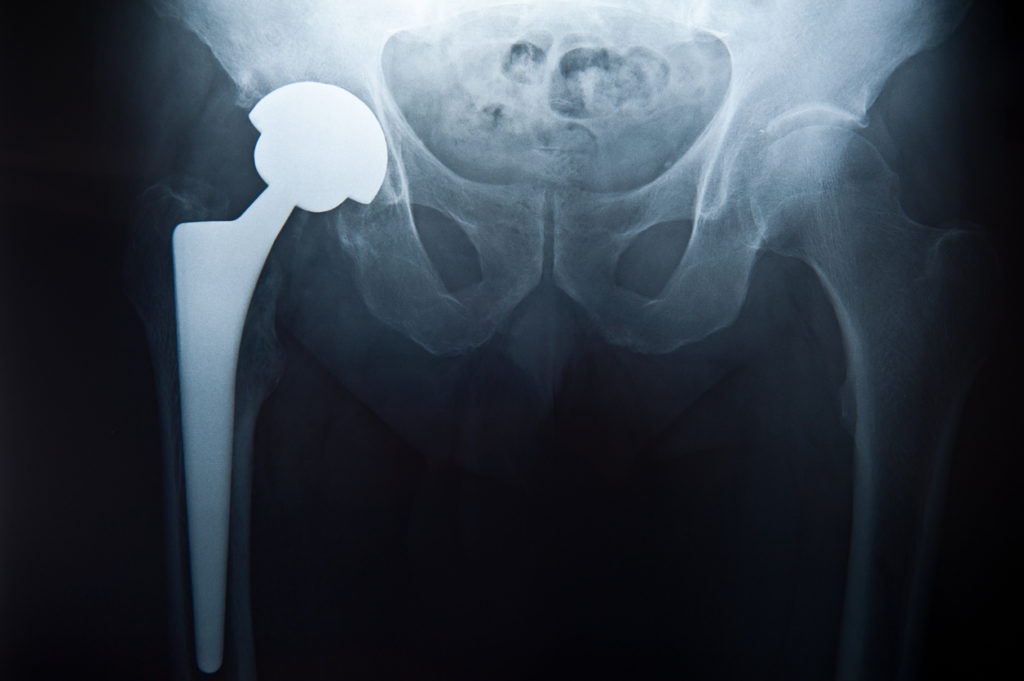
At Redwood Orthopaedic Associates, we perform a total hip replacement to remove the damaged parts of the hip and replace them with artificial components. This surgery is very successful and allows the patient to return to most activities without pain.
Do I Need Hip Replacement Surgery?
The most common cause of chronic hip pain and damage is arthritis, in this case osteoarthritis, rheumatoid arthritis, and traumatic arthritis.
- Osteoarthritis — Most all of us have some degree of this “wear-and-tear” arthritis, as we get older. In the hips, osteoarthritis damages the slick cartilage that covers the ends of the femur and the inside of the hip socket.
- Rheumatoid Arthritis — Rheumatoid arthritis creates inflammation that erodes cartilage and bone in the hips.
- Post-Traumatic Arthritis — If you’ve had a serious hip injury or fracture, the cartilage could have been damaged, leading to pain and stiffness over time.
- Osteonecrosis — Sometimes a hip dislocation or fracture can limit the blood supply to the femoral head, which causes the surface of the bone to collapse.
- Childhood Hip Disease — In rare cases, children have hips that didn’t develop normally. Even if the hips were successfully treated during childhood, these conditions will often lead to arthritis later in life.
Would I Be a Good Candidate for Hip Replacement Surgery?
Most people don’t make a knee jerk decision to go have a hip replaced. It usually is a long process of dealing with and managing pain, of missing out on certain favorite activities such as hiking or playing tennis, and trying other treatments such as cortisone injections or arthroscopic procedures to try and clean out the hip joint. Finally, when chronic pain begins to impact daily life, hip replacement begins to enter the person’s thinking. People who opt to have a total hip arthroplasty often have these symptoms:
- Hip pain that limits everyday activities, such as walking or bending
- Hip pain that continues even when the hips are not carrying any load, such as when sleeping
- Stiffness in the hip that limits the ability to move or lift the leg
- Inadequate pain relief through physical therapy, anti-inflammatory drugs, or walking supports
How is Hip Replacement Surgery Performed?
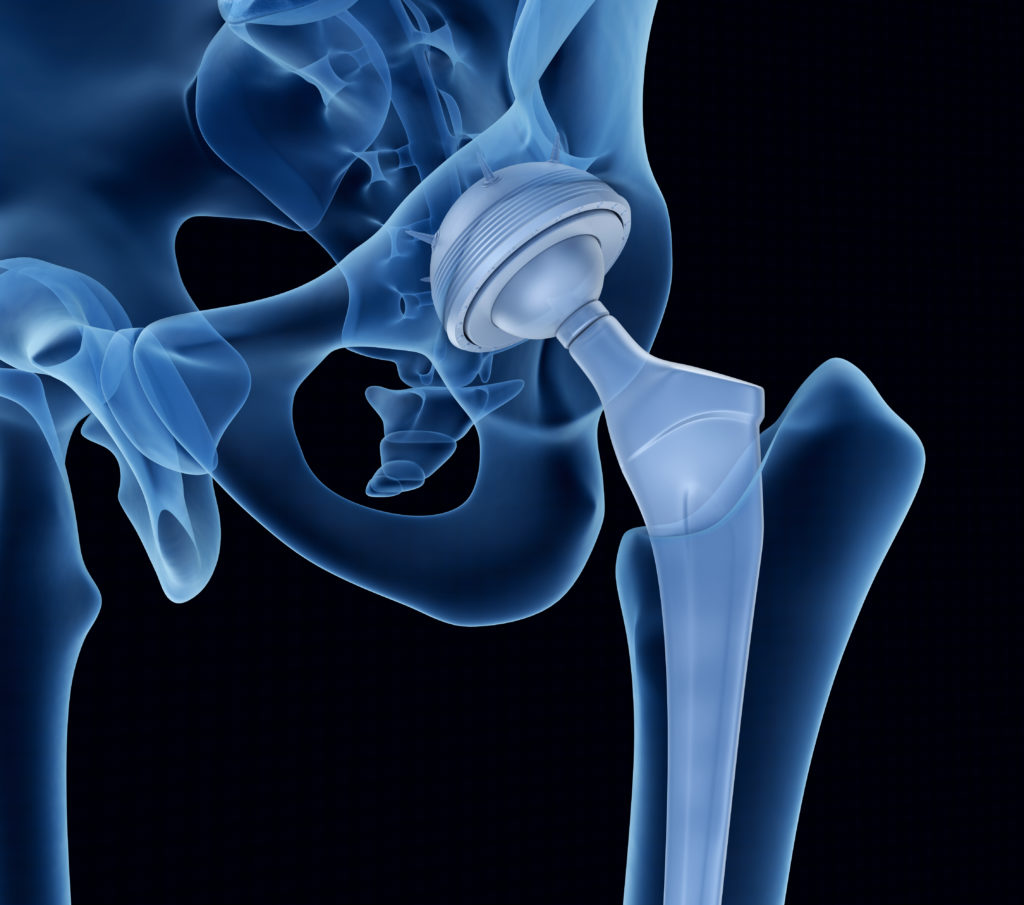
A total hip arthroplasty contains two main components: the ball component that replaces the femur head and the socket. The ball is made of highly polished metal or ceramic. The socket component is made from plastic, ceramic or metal.
Your Redwood Orthopaedic Associates surgeon begins this procedure by making an incision over the front or side of your hip to gain access to the hip. The surgeon then removes diseased and damaged bone and cartilage, leaving healthy bone. The artificial cup is first placed in the hip socket, either with cement or screws. Next, the end of the femur is cut off and a stem is placed down into the femur. This stem may either be cemented or “press fit” into the bone. A metal or ceramic ball is then placed on the upper part of the stem, replacing the femur head. A plastic, ceramic, or metal spacer is inserted into the artificial socket before the new artificial femur head is placed into the new socket to create a smooth gliding surface. This ends the procedure and the incision is closed with stitches or staples.
Hip Replacement Recovery
The most important facet of early recovery is the prevention of blood clots in your legs. To prevent these from developing, you’ll be encouraged to sit up and then walk with crutches or a walker, in most cases the same day as your surgery. We’ll have you in compression stockings or an inflatable air sleeve on your lower legs. This pressure keeps blood from pooling in the leg veins, reducing the chance a clot will form. You will also be placed on an oral blood thinner. You may need to take this for several weeks. It’s important to regain the use of your hip and the surrounding muscles. To do this, you’ll be teamed with a physical therapist. You’ll learn how to use walking assistance devices such as crutches or a walker. Your therapist will help you build back strength and mobility in the hip. You’ll have a follow-up appointment with us in 6-12 weeks. If everything is healing well, you’ll be cleared to resume normal activities, although you may not feel you’re fully recovered until 6-12 months.
Will I Need Physical Therapy After A Total Hip Arthroplasty?
Yes. As mentioned above, your physical therapist will help you strengthen the muscles around the hip with various exercises. Another goal will be to return and extend flexibility.
What Results Can I Expect?
Most patients are thrilled with their new hip. Pain should be minimal or completely gone. You’ll be able to hike, swim, ride a bike, even return to the golf course. But it will probably be wise to stay away from high-impact activities, such as running or playing volleyball.
The most common comment we hear from hip replacement patients is, “Why did I wait so long to have this done?”
What are the Risks of Hip Replacement Surgery?
Complications with hip arthroplasty surgery are rare, occurring in less than two percent of patients. These are the typical possible complications:
- Infection — Infection can occur superficially in the wound or deep around the prosthesis. It can even occur years later, as infection from elsewhere in your body can spread to your new hip.
- Blood Clots — Blood clots in the leg veins or pelvis are one of the most common complications. If a clot breaks free and travels to your lungs, it can be life threatening.
- Leg-Length Difference — One leg may feel longer or shorter than the other after hip replacement. This may be a byproduct of maximizing stability or biomechanics in the hip.
- Dislocation — The risk of the ball leaving the new hip socket is greatest in the first few months after surgery, when your tissues are not fully healed and strong.
- Loosening and Wear — Over time, your hip prosthesis may wear out or loosen. If the looseness eventually leads to pain, a revision surgery could be necessary.
How Long Before I Can Get Back to Normal Activities After My Hip Replacement Surgery?
- Driving? You won’t be able to drive for at least 4 weeks.
- Walking? You’ll be restricted to the use of a walker or crutches for 2-3 weeks. You can then switch to a cane outdoors and no support around the house. It will take around 3 months before you fully walk without assistive devices.
- Showering? You may shower 4 days after your surgery.
- Work? If your job is sedentary, you can probably return to work within 1 month. If your job is active, you may need up to 3 months.
- Sex? Most patients can resume sexual activity in 6-8 weeks.
How Long Will My New Hip Last?
Up to 95 percent of total hip replacements should last 15 years or longer. Lifespans are increasing, however, so this number should keep expanding.
Redwood Orthopaedic Surgery Associates proudly provides patients from Santa Rosa, CA and surrounding areas with hip replacement surgery. Contact us at (707) 544-3400 or fill out a Contact Form here.

